To Keep Everybody Safe Sandra Keogh
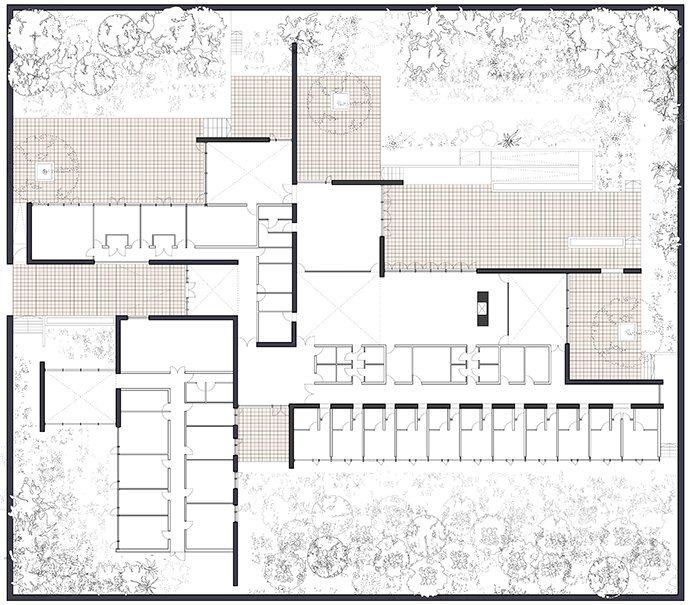
Niall McLaughlin and Yeoryia Manolopoulou speak to Sandra Keogh, the Person in Charge of The Orchard Alzheimer’s Respite Centre in Dublin, which was designed by Niall McLaughlin Architects for the Alzheimer Society of Ireland (and is the starting point for our animation). Sandra has been in charge of the Orchard since 2015. She previously worked extensively with people with intellectual disabilities and dementia; including at the first purpose-built unit for the care of people with intellectual disabilities and Alzheimer’s Disease in Ireland.
Sandra explains that The Orchard offers two forms of care; daycare and respite care. Daycare is usually provided in the middle stages of Alzheimer’s progression, and offers the family a break, or the ability to work during the day, while the person with dementia socialises and engages in stimulating activities. Respite care is typically provided to people in the latter stages of the disease, providing a break for their family from the ongoing provision of care.
Sandra discusses how a balance is struck between these distinct forms of care in the day-to-day running of The Orchard. Niall asks if, due to their differing rhythms, requirements and aspirations, she feels they should be located in separate buildings. Sandra agrees that the care needs are very different, but says that ideally, the daycare and respite clients would be drawn from the same cohort of people, who are familiar with the building and the staff. However, she suggests that some degree of physical separation would be desirable, perhaps with a fully-overlooked garden as a shared space.
This conversation highlights the predicament of 'designing for dementia' as a specialist need; as the needs and capabilities of someone with dementia will change and develop over time. Sandra acknowledges that it's very difficult, and that the range of care needs is very wide. She proposes that ideally any building with dementia could be designed to allow for this progression, suggesting that there could be a long-term care element within the same environment. She proposes a campus-type model comprised of daycare, respite and long term care – with some physical separation between them – and the same team of nurses/carers throughout. This would allow clients and their families to form long-term relationships with the caring team.
Niall raises the change in caring approach from the more voluntary-based system he found when first meeting the Alzheimer’s Society of Ireland in 1999, to the highly-professional, regulated model in place now. He asks Sandra if she believes this has placed limitations on creativity in care. She points out that some volunteers still work within the organisation – driving, befriending clients, leading sing-songs. Sandra agrees that there are now many legislative standards to be met, but says that the Health and Information Quality Authority set these out 'to keep everybody safe'. She is categorical in her belief that care is better now: creativity may be restricted, but there are fewer variations and failures in care provision.
Yeoryia points out that ‘design for dementia’ often focuses on the needs of the clients, and asks Sandra how a building can be designed to meet the needs of the staff. Sandra cites pragmatic considerations: wide doorways that hospital beds can fit through if required; garden areas that are thoroughly visible from within the building; and administrative offices that are separate from the care environment, to minimise distractions. She recommends that the nurses station is very open, overseeing as much of the building as possible. Yeoryia asks if there could be more shared social spaces between carers and clients, but Sandra stresses the need for a separate staffroom, to allow staff a break from the day. However, she would like a space in which social cooking activities could take place.
Yeoryia questions whether there could be more personalisation within bedrooms; if clients could store some of their personal objects at The Orchard for their visits. She notes the advantages of objects for navigation and comfort, but Sandra says this would be too difficult to manage: storage space is at a premium, and personal things can easily go missing. She agrees that personalisation can enhance a person’s experience of their space, but argues that it’s more appropriate to long term care.
The conversation turns to the gardens, which are currently gated off. All agree that ideally, these would be accessible and open. Niall asks how they could have been designed differently to facilitate this. Sandra says that, while dementia alone shouldn’t preclude someone from enjoying an enclosed garden, the age profile of people with dementia means that there are often other conditions which affect mobility and design should consider this. However, she highlights the positive contribution of the garden to The Orchard; and tells a story of one client who used to come for daycare specifically when the gardeners were on site, so he could feel that he was working the garden.
To conclude the conversation, Sandra outlines what she sees as the successes of the building: the communal spaces can accommodate large groups, or, through the closure of the separating doors, can facilitate separate concurrent activities. She praises the ability of building to adapt from day to night, describing how different sitting rooms are used and lit depending on the time of day. She describes the dining room as social hub: "it has a real buzz when you come into it at a mealtime".